Zealand Pharma, a Danish biotech company, is aiming to revolutionize the obesity treatment market with what it calls the “next generation” of weight loss drugs. Competing against major players like Novo Nordisk and Eli Lilly, Zealand Pharma’s CEO, Adam Steensberg, expressed optimism about the company’s experimental drugs that could set new standards for weight management, particularly with its amylin analog candidate, Petrelintide. Steensberg referred to Petrelintide as their “crown jewel,” positioning it as an alternative to the increasingly popular GLP-1 treatments, such as Novo Nordisk’s Wegovy and Eli Lilly’s Zepbound.
The Promise of Petrelintide and Dapiglutide
While Zealand Pharma has already reported positive results from early-stage trials of Dapiglutide, a GLP-1/GLP-2 receptor dual agonist, the company’s real focus is on Petrelintide, which offers a novel approach by mimicking the hormone amylin. Amylin, co-secreted with insulin, helps regulate feelings of fullness (satiety), a mechanism different from GLP-1 treatments that suppress appetite by mimicking gut hormones. This differentiation is key, as Petrelintide aims to offer significant weight loss with fewer side effects and reduced muscle loss—common concerns associated with current GLP-1 treatments.
According to Steensberg, the goal is to offer patients a more “pleasant experience” with long-term treatment possibilities. Amylin analogs like Petrelintide are emerging as a new category in obesity treatment, with the potential to become a foundational therapy in the coming years.
Strong Early Results and Growing Competition
In June 2024, Zealand Pharma announced promising results from a phase 1b trial of Petrelintide, which demonstrated an average body weight reduction of up to 8.6% over a 16-week course. The company believes this robust data supports Petrelintide as a viable alternative to GLP-1 treatments, particularly for those who struggle with their side effects.
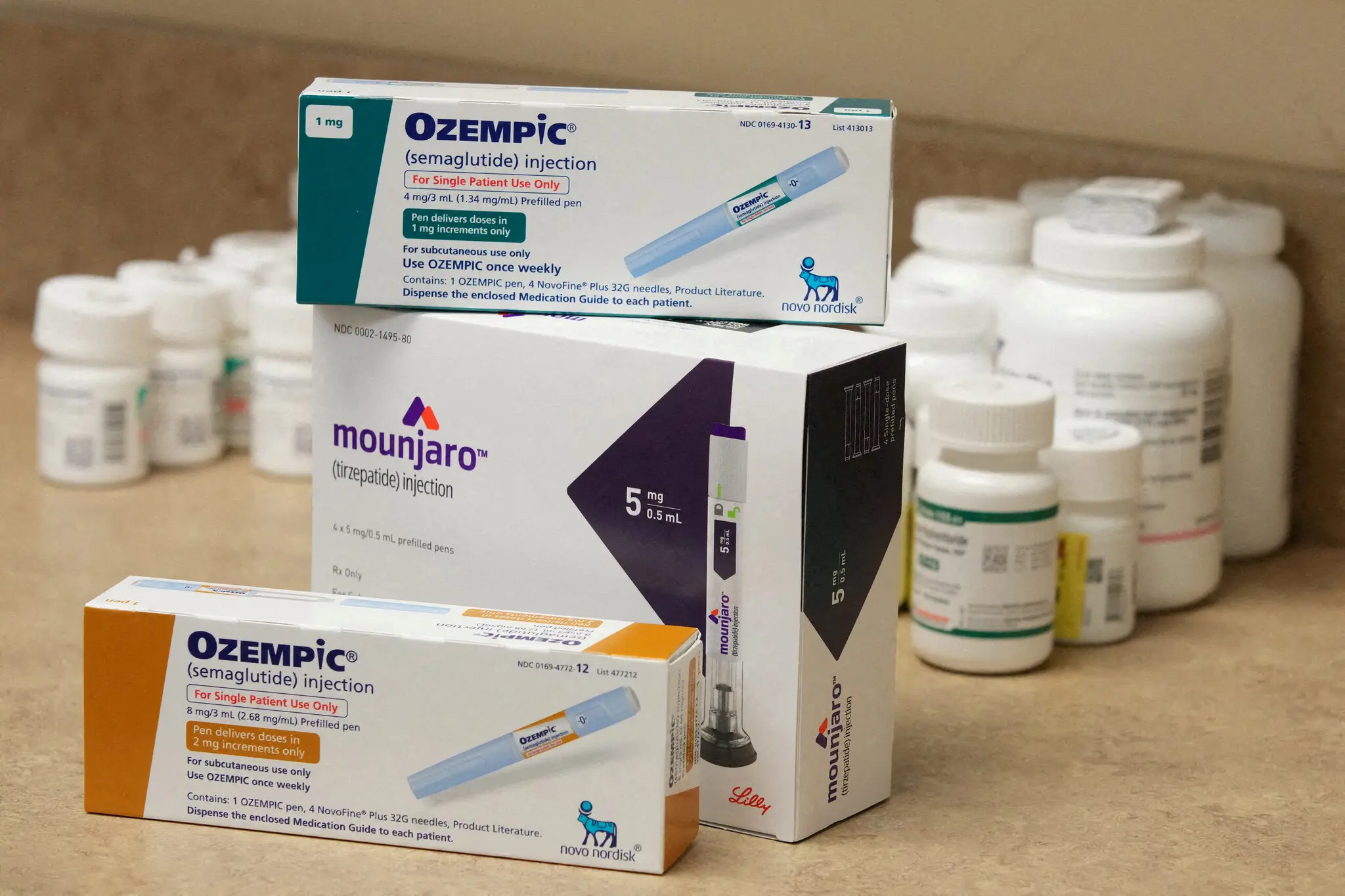
Novo Nordisk, which currently dominates the obesity market, is also working on its own amylin-based therapy by combining semaglutide (the active ingredient in Wegovy) with amylin analog Cagrilintide in a candidate drug called CagriSema. This further highlights the growing interest in amylin-based therapies within the competitive obesity treatment landscape.
Zealand Pharma’s smaller size presents a challenge in competing with the pharmaceutical giants. Emily Field, head of European pharmaceuticals research at Barclays, noted that while Zealand Pharma’s developments are promising, the company will likely need a larger pharmaceutical partner to scale its operations effectively.
Searching for a Global Pharma Partner
Zealand Pharma, which has seen its share price more than double this year due to excitement around its obesity drugs, is now actively seeking a global pharmaceutical partner to help bring its treatments to market. Steensberg acknowledged that despite the company’s recent $1 billion capital raise, partnership is essential for the next phase of development, particularly as both Petrelintide and Dapiglutide move into phase 2 trials in 2024 and 2025.
With rising competition, including established players like Novo Nordisk and Eli Lilly and an estimated $200 billion market by 2030, partnering with a global firm would provide Zealand Pharma with the resources necessary to scale production and marketing efforts.
Future of Obesity Treatment and Market Fragmentation
The obesity drug market is expected to become increasingly fragmented as different pharmaceutical companies target specific segments and patient needs. Analysts believe that focusing on niche areas, such as treatments that reduce muscle loss, will help smaller companies like Zealand Pharma carve out space alongside the market leaders. As demand for these treatments continues to surge globally, companies are racing to create the next big breakthrough in weight management.
Zealand Pharma’s strategic focus on amylin analogs, coupled with its search for a strong pharmaceutical partner, positions the company to make a significant impact in the coming years. Steensberg remains optimistic, viewing their developments as “an attractive opportunity” for potential partners and asserting that amylin analogs could become a first-line therapy in the near future.
Conclusion
Zealand Pharma’s innovative obesity drug candidates, particularly Petrelintide, hold great promise in reshaping the future of weight management treatments. As the company advances its clinical trials and seeks a global pharmaceutical partner, it faces both opportunities and challenges in an increasingly competitive and lucrative market. With the growing demand for effective and tolerable weight loss solutions, Zealand Pharma’s next-generation treatments may very well play a pivotal role in the future of obesity care.